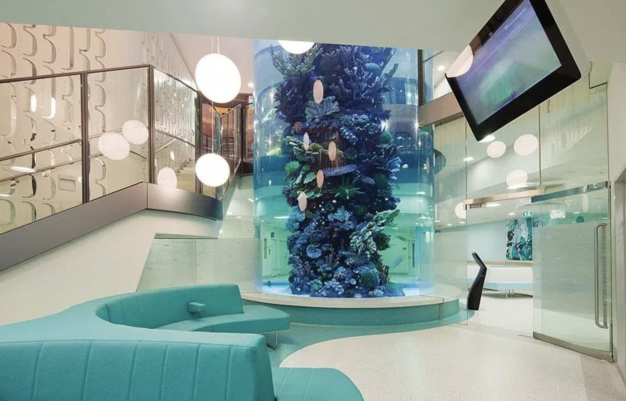
Aquariums, meerkats and gaming screens: how hospital design supports children, young people and their families
Every time you take your child to the emergency department or a loved one to a mental health outpatient appointment, the very building and spaces you encounter will have been designed, for a number of reasons.
Not only will these spaces be functional, their designs encourage patients to seek help or act to relieve stress. This type of design looks at how buildings and landscapes improve mental health.
By Stephanie Kathleen Liddicoat, Lecturer, Architectural Design, Swinburne University of Technology; Eóin Killackey, Professor of Functional Recovery in Youth Mental Health, Centre for Youth Mental Health, University of Melbourne, and Paul Benjamin Badcock, Senior Lecturer, University of Melbourne
Just as evidence-based medicine uses evidence to inform clinical practice, evidence-based design informs architects and other designers how to design our hospitals, surgeries and clinics to improve patient care.
So, how does this type of design influence how we plan and build spaces with mental health and well-being in mind?
Show me the evidence
Evidence-based design, which has become more popular in the past three decades, assumes an intimate connection between health-care facilities and patient well-being.
It uses a wide range of measures to assess how someone’s psychological response to a built environment influences physiological, cognitive and functional outcomes.
The aim is to provide evidence for what works and what doesn’t to improve recovery from mental ill-health, by reducing hospital stays, distress, anxiety and aggression, while promoting staff performance and retention.
 This interactive gaming screen at Monash Children’s Hospital reduces the anxiety of waiting for an appointment, while encouraging socialisation.
This interactive gaming screen at Monash Children’s Hospital reduces the anxiety of waiting for an appointment, while encouraging socialisation.
Ouva
For instance, one key piece of research found people recovered faster after surgery, and used fewer painkillers, if their hospital bed overlooked a natural scene (like a garden) rather than a brick wall.
Read more:
Green for wellbeing – science tells us how to design urban spaces that heal us
Over the same time as evidence-based design has grown in popularity, there has been a growing emphasis in mental health on providing user-friendly services and improving user and carer experiences.
In Australia, this has become particularly apparent in youth mental health.
According to the World Health Organisation’s guidelines, quality, youth-friendly health services need to be “accessible, acceptable and appropriate”, and offered in the right place, at the right time and price. They must also be in the “right style” for young people, their supporters and the broader community.
Here are two principles of how this works when designing for mental health and well-being.
1. Involve young people and their carers early in the design process
If you include young people’s needs and perspectives when designing a mental health service, this improves their engagement in that service, the quality of care and their health.
For most young people, their relationships with family members and other primary carers also play a key role in their mental health and recovery.
So, providing appropriately designed spaces for both young people and their carers is critical.
 The Royal Children’s Hospital, Melbourne: hospital or art gallery?
The Royal Children’s Hospital, Melbourne: hospital or art gallery?
Bates Smart
On a practical level, this might mean providing comfortable spaces for young people, their supporters and clinicians to meet; providing privacy so they can’t be overheard or seen; or designing waiting areas for small groups.
For instance, Melbourne’s Orygen youth mental health facility, which opened in 2018, consulted extensively with young people, family and carers throughout the design process.
When young people enter the facility, they are greeted by a trained concierge rather than a formal reception area, and provided with a range of seating options, both inside and out.
Meanwhile, family members can take a leisurely stroll along several landscaped walking tracks while their loved one has their appointment.
These principles have also been applied to other health facilities for children, not just those specialising in mental health.
For instance, Monash Children’s Hospital has a large interactive gaming screen, where children and parents can pass the time waiting for their appointment.
This reduces the anxiety of waiting for an appointment, while encouraging the positive effects of socialisation within and between families.
2. Change people’s expectations of care
Some people find it stigmatising to access mental health care. But the physical setting can help people reframe their expectations about what their care might entail.
So, we move away from expectations of “control” or “incarceration” to expectations of comfort, well-being and care.
This shift helps people better engage with health-care professionals, improving their experiences of care and their well-being.
 Look, meerkats! Melbourne’s Royal Children’s Hospital has a permanent meerkat enclosure, much to the delight of children and their carers.
Look, meerkats! Melbourne’s Royal Children’s Hospital has a permanent meerkat enclosure, much to the delight of children and their carers.
Green and Dale Associates
So, the environment must be comfortable, familiar and de-institutional. It must reduce the visibility of security and safety features, while providing activities that support well-being and mindfulness, such as courtyards, communal gardens, natural environments, art-based activities and social opportunities.
 These huge musical instruments are part of London’s Great Ormond Street Hospital’s ‘lullaby factory’.
These huge musical instruments are part of London’s Great Ormond Street Hospital’s ‘lullaby factory’.
Studio Weave
Reframing expectations is also critical when designing more general children’s facilities.
For instance, Melbourne’s Royal Children’s Hospital has a meerkat enclosure, interactive gaming screen, sculptures, an aquarium, and a children-only activity room.
These types of features give the impression of the hospital, not as a frightening or intimidating place, but of an exciting hub of activity with things to do and friends to meet.
Likewise, London’s Great Ormond Street Hospital for Children has been transformed into a “lullaby factory”. Here, giant musical phones and instruments weave their way between hospital buildings, playing music to captivated children and families.
What can we expect in the future?
Despite these encouraging efforts, there is still a long way to go before the influence of evidence-based design on mental health care is truly felt.
Despite its broad adoption, it is critiqued for being too rigid, using broad or ill-defined research terms, or for claiming connections between an isolated variable in the environment and a behaviour, when such straight-forward connections are not guaranteed.
So we need to commit more time, energy, resources, and transdisciplinary collaborations in this crucial area of mental health service delivery to address these concerns.
Read more:
To really fix Victoria’s mental health system, we’ll need to bridge the state/Commonwealth divide
In positive news, the recent interim report from Victoria’s mental health royal commission recognises the importance of appropriately designed mental health-care facilities.
It recommends new acute mental health beds that are “contemporary, co-designed with people with lived experience”.
It’s important these new facilities and services thoughtfully respond to the mental health needs of children and young people, to ensure accessible and appropriate support when they need it most.
This article is the latest in The Conversation’s Designing Hospitals series, which explores how architecture and design shape our hospitals and medical centres. This article looks at how good design affects mental health and well-being, particularly in young people.
Read the other Designing Hospitals articles:
From army barracks to shopping malls: how hospital design has been a matter of life and death
Making space: how designing hospitals for Indigenous people might benefit everyone
![]()
Stephanie Kathleen Liddicoat, Lecturer, Architectural Design, Swinburne University of Technology; Eóin Killackey, Professor of Functional Recovery in Youth Mental Health, Centre for Youth Mental Health, University of Melbourne, and Paul Benjamin Badcock, Senior Lecturer, University of Melbourne
This article is republished from The Conversation under a Creative Commons license. Read the original article.




